📅 Updated: April 2026 | ⏱ 14-minute read | ✅ Medically & Legally Reviewed
Introduction
Mesothelioma Surgery Options 2026 Surgery offers mesothelioma patients something that chemotherapy and immunotherapy alone cannot: the physical removal of tumors from the body. For eligible patients, it represents the best chance of long-term survival, and in combination with chemotherapy and/or immunotherapy, surgical treatment has helped mesothelioma patients achieve survival times that were unthinkable just a decade ago.
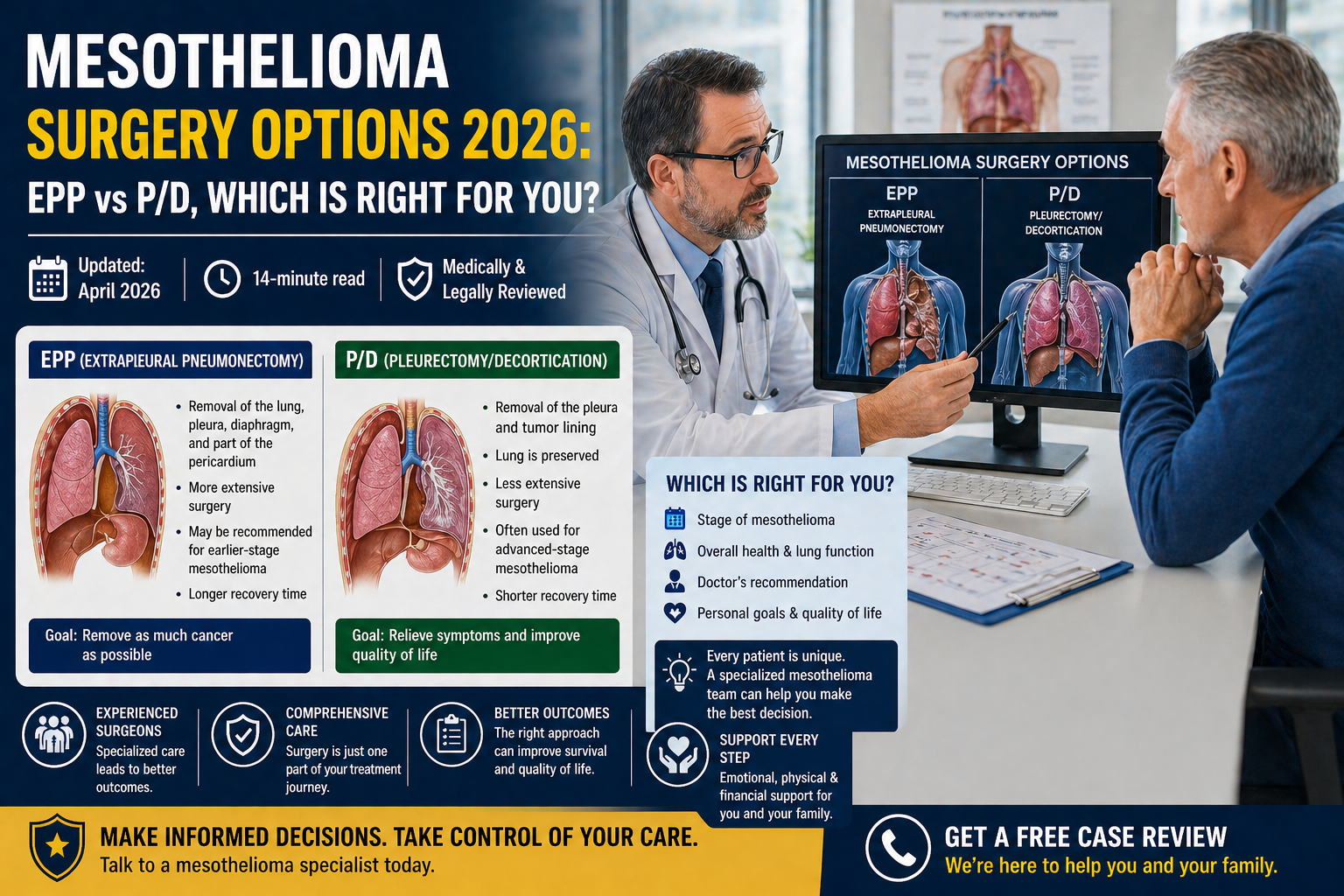
But mesothelioma surgery is not one procedure. It is a family of surgical approaches, each with different risks, different recovery profiles, different eligibility requirements, and meaningfully different long-term outcomes. The two primary operations for pleural mesothelioma, Extrapleural Pneumonectomy (EPP) and Pleurectomy/Decortication (P/D), are not interchangeable. Choosing between them, or being told you’re not a candidate, is one of the most consequential decisions in a mesothelioma patient’s treatment journey.
And in 2026, the science has shifted significantly. A landmark study published in The Annals of Thoracic Surgery in February 2026, from the Icahn School of Medicine at Mount Sinai, one of the world’s leading mesothelioma centers, demonstrated 0% in-hospital mortality and 0% 30-day mortality for carefully selected P/D patients. These results directly challenge earlier data suggesting surgery was too risky for most patients.
This guide covers everything you need to know: what each procedure involves, how they compare, who qualifies, what survival rates look like in 2026, how peritoneal surgery works, and how surgery affects your legal compensation rights.
Why Surgery Matters for Mesothelioma
Mesothelioma is a cancer of the mesothelium, the protective lining surrounding the lungs (pleura), abdomen (peritoneum), and heart (pericardium). Unlike many solid tumor cancers where surgery simply removes a discrete mass, mesothelioma typically spreads as a sheet of tumor tissue across the pleural surface, making complete surgical removal technically demanding and highly specialized.
Despite this challenge, surgery remains the single most powerful tool for extending survival in eligible mesothelioma patients. The data is consistent:
| Treatment Approach | Median Survival |
|---|---|
| Chemotherapy alone | ~12–14 months |
| Immunotherapy alone | ~18.1 months |
| Surgery + Chemotherapy (multimodal) | ~22–31 months |
| CRS-HIPEC (peritoneal) | ~44–53 months |
The gap between surgery-inclusive and surgery-exclusive treatment is significant, and it widens further at specialized, high-volume mesothelioma centers where surgical expertise directly translates into better outcomes.
The Two Primary Mesothelioma Surgery Options for Pleural Disease
Surgery Option 1: Pleurectomy/Decortication (P/D)
Pleurectomy/Decortication is a lung-sparing surgery, and as of 2026, it is the preferred surgical approach at most leading mesothelioma centers worldwide.
What it involves:
- Removal of the pleural lining (the mesothelium covering the lung surface and chest wall) on the affected side
- Removal of all visible tumor nodules from the pleural surface, chest wall, and mediastinum
- The lung itself is preserved, it remains in the body after surgery
- The diaphragm and pericardium may be partially resected in an “extended P/D” if tumor involvement requires it
What is NOT removed:
- The affected lung
- Standard heart lining (pericardium) unless required by tumor extent
Surgical time: Typically 4–8 hours, depending on tumor extent.
The 2026 Mount Sinai Study, Why P/D Is Now Definitively Supported
The most important surgical research publication of 2026 comes from Dr. Raja M. Flores and his team at the Icahn School of Medicine at Mount Sinai, one of the highest-volume mesothelioma surgery programs in the United States.
Published in The Annals of Thoracic Surgery (February 2026), the study analyzed outcomes for 71 mesothelioma patients who underwent P/D between 2015 and 2021 under rigorous patient selection protocols.
Results:
| Outcome Metric | Mount Sinai P/D Study | MARS2 Trial (UK) |
|---|---|---|
| In-hospital mortality | 0% | 4% |
| 30-day mortality | 0% | 4% |
| 90-day mortality | 4.2% | 9% |
| PET/CT imaging required | Yes, 100% | Not mandated |
| Sarcomatoid patients included | No | Yes (5%) |
| Extended P/D rate | Rare (tailored approach) | 89% |
The MARS2 trial, a UK-based study conducted over the same time period, had concluded that P/D surgery led to worse outcomes than chemotherapy alone, sparking significant debate about whether surgery should be offered to mesothelioma patients at all.
The Mount Sinai study demolishes that conclusion, by demonstrating that patient selection and surgical technique are the critical variables, not surgery itself.
“Our findings show that pleurectomy/decortication can be done safely when patients are carefully selected and surgery is tailored to balance tumor removal with the patient’s ability to tolerate aggressive treatment. Surgery should remain part of the conversation for mesothelioma treatment and can lead to long-term survivorship.”
, Dr. Raja M. Flores, MD, Professor of Surgery & Chair of Thoracic Surgery, Mount Sinai Health System (February 2026)
What this means for patients: If you or a loved one has been told that surgery “isn’t an option”, particularly by a general oncologist citing the MARS2 trial, these 2026 findings strongly support seeking a second opinion from a mesothelioma surgical specialist.
07:45
Surgery Option 2: Extrapleural Pneumonectomy (EPP)
Extrapleural Pneumonectomy is the more radical of the two primary surgical approaches. It removes far more tissue and carries a higher surgical risk, but in carefully selected cases, it may achieve more complete tumor removal.
What it involves:
- Complete removal of the affected lung
- Removal of the pleural lining on the affected side
- Removal of the diaphragm on the affected side (replaced with a prosthetic patch)
- Removal of the pericardium (the lining around the heart) on the affected side (replaced with a prosthetic patch)
Surgical time: Typically 6–10 hours.
Recovery: Longer and more physically demanding than P/D, patients lose an entire lung and must adapt to breathing with one lung for the rest of their lives.
EPP vs P/D, The Complete 2026 Comparison
| Factor | EPP (Extrapleural Pneumonectomy) | P/D (Pleurectomy/Decortication) |
|---|---|---|
| Lung preserved? | ❌ No, entire lung removed | ✅ Yes, lung is preserved |
| Structures removed | Lung, pleura, diaphragm, pericardium | Pleural lining + visible tumors |
| Surgical mortality | ~5–7% | ~1–4% (0% at top centers in 2026) |
| Recovery time | 8–12 weeks | 4–8 weeks |
| Hospital stay | 10–14 days | 7–10 days |
| Long-term lung capacity | Significantly reduced (one lung) | Better preserved |
| Best candidate | Younger, excellent function, early-stage, epithelioid | Broader candidate pool |
| Median survival (multimodal) | 12–22 months | 16–31 months |
| Quality of life post-op | Lower (one lung) | Better |
| Risk of local recurrence | Lower | Slightly higher |
| Currently preferred? | Less commonly now | ✅ Yes, increasingly preferred worldwide |
Which Is Better, EPP or P/D?
The trend in 2026 is clear: P/D has become the preferred surgical option at the majority of major mesothelioma centers. Here’s why:
- Lower surgical mortality, the Mount Sinai study showed 0% 30-day mortality with properly selected P/D patients vs. 4–7% historically for EPP
- Better quality of life, patients keep their lung; breathing function is significantly better after recovery
- Comparable or superior survival, multiple studies now show P/D achieves equivalent or better long-term survival compared to EPP in most patient populations
- Broader eligibility, patients who don’t meet EPP eligibility criteria (due to age, lung function, or health status) may still be P/D candidates
However, EPP still has a role in specific clinical situations, particularly for younger patients with exceptional health, very early-stage disease, and cases where the tumor has extensively infiltrated the lung parenchyma itself. The decision must be made by an experienced mesothelioma surgeon evaluating your specific case.
Who Is a Candidate for Mesothelioma Surgery?
Surgery is not appropriate for every patient, but more patients qualify than many general oncologists realize. Eligibility depends on multiple factors that must be carefully evaluated together.
Factors That Favor Surgical Candidacy
| Factor | Favorable for Surgery |
|---|---|
| Cell type | Epithelioid (responds best to surgery) |
| Disease stage | Stage 1 or 2 (localized disease) |
| Performance status | ECOG 0–1 (active, minimal symptoms) |
| Age | Under 70 (generally), though older patients are evaluated individually |
| Lung function | Adequate FEV1 and DLCO on pulmonary function tests |
| Cardiac function | Normal or near-normal heart function |
| Disease extent | Confined to one side of the chest, no distant metastasis |
| Lymph node status | No contralateral (opposite side) lymph node involvement |
Factors That Generally Exclude Surgery
- Sarcomatoid cell type, responds poorly to surgery; most centers exclude sarcomatoid patients from surgical protocols (as the Mount Sinai study showed, only 2.8% of their surgical patients had sarcomatoid histology)
- Stage 3–4 disease, extensive chest wall invasion, bilateral disease, or distant metastasis
- Poor performance status, ECOG 2+ indicates insufficient reserve for major surgery
- Inadequate lung or cardiac function, particularly critical for EPP where one lung is removed
- Significant comorbidities, uncontrolled diabetes, renal failure, severe cardiovascular disease
The Critical Importance of Surgical Eligibility Assessment at a Specialist Center
This cannot be overstated: A patient told by a community hospital or general oncologist that they are “not a surgical candidate” should always seek a second opinion at a high-volume mesothelioma surgical center.
Eligibility assessment requires:
- High-resolution CT and PET/CT imaging reviewed by mesothelioma-experienced radiologists
- Pulmonary function testing including quantitative ventilation-perfusion (V/Q) scanning
- Cardiac evaluation
- Multidisciplinary tumor board review, surgeons, medical oncologists, radiation oncologists, and pathologists discussing the case together
Centers that see hundreds of mesothelioma surgical cases routinely identify candidates that lower-volume centers miss. Patient selection is itself a specialized skill.
Mesothelioma Surgery Survival Rates 2026
| Surgery Type | Median Survival | 2-Year Survival | 5-Year Survival |
|---|---|---|---|
| P/D alone | ~16 months | ~40% | ~10% |
| P/D + Chemotherapy | ~20–26 months | ~50–55% | ~15–20% |
| P/D + Chemo + Radiation (trimodal) | ~26–31 months | ~55–65% | ~20–25% |
| EPP + Chemotherapy | ~12–19 months | ~41% | ~10–15% |
| EPP + Chemo + Radiation (trimodal) | ~22 months | ~45% | ~12–18% |
Sources: Annals of Thoracic Surgery, 2026; Mesothelioma Guide survival data; NCI SEER database; published peer-reviewed studies
Key insight from the data: P/D combined with chemotherapy and radiation (trimodal therapy) now consistently outperforms EPP-based multimodal therapy in most published series, reinforcing P/D’s status as the preferred surgical approach in 2026.
Surgery for Peritoneal Mesothelioma, CRS-HIPEC
For peritoneal mesothelioma, which affects the abdominal lining rather than the lung lining, a completely different surgical approach is used: Cytoreductive Surgery (CRS) combined with Hyperthermic Intraperitoneal Chemotherapy (HIPEC).
What Is CRS-HIPEC?
Phase 1, Cytoreductive Surgery (CRS)
The surgeon removes all visible tumor nodules from the peritoneal surfaces and abdominal organs. The goal is complete cytoreduction (CC-0 or CC-1, no visible or only microscopic residual tumor).
Phase 2, HIPEC
Immediately following surgery, the entire abdominal cavity is filled with a heated chemotherapy solution (typically cisplatin at 41–43°C) and circulated for 60–90 minutes. The heat enhances drug penetration into residual microscopic cancer cells while limiting systemic exposure.
Total procedure time: 8–14 hours.
CRS-HIPEC Survival Data 2026
| Patient Group | Median Survival | 5-Year Survival |
|---|---|---|
| Optimal CRS-HIPEC candidates | 44–53 months | 47–65% |
| Epithelioid + complete cytoreduction (CC-0) | Up to 80 months (repeat HIPEC) | 65%+ |
| Chemotherapy alone (peritoneal) | ~12–15 months | ~5% |
The 65% 5-year survival rate for optimal peritoneal mesothelioma patients treated with CRS-HIPEC is one of the most remarkable statistics in oncology, transforming what was once a universally fatal diagnosis within 12 months into a disease with genuine long-term survivorship potential.
Multimodal Treatment, Combining Surgery With Other Therapies
Surgery is most effective when used as part of a multimodal treatment plan:
Neoadjuvant Therapy (Before Surgery)
Chemotherapy or immunotherapy given before surgery can:
- Shrink tumors, making surgical removal more complete
- Test whether the tumor is responsive to systemic therapy
- Eliminate microscopic disease before the surgical field is opened
Active 2026 trial: The durvalumab + tremelimumab ± chemotherapy neoadjuvant trial at MD Anderson Cancer Center is directly testing whether immunotherapy before surgery improves outcomes for resectable pleural mesothelioma.
Adjuvant Therapy (After Surgery)
Chemotherapy and/or radiation given after surgery to:
- Eliminate residual microscopic disease at the surgical margins
- Reduce local recurrence risk
- Improve long-term survival in combination with surgical resection
Intraoperative Radiation (IORT)
Some centers deliver targeted radiation to the surgical field during surgery, reaching tumor cells directly while the chest is open and before normal tissue is restored. Available at select high-volume centers.
Photodynamic Therapy (PDT)
Light-activated drugs are administered and then activated by surgical light during the operation, selectively destroying residual cancer cells. Being studied as an intraoperative adjunct in several active trials.
Mesothelioma Surgery Recovery, What to Expect
P/D Recovery Timeline
| Timeframe | What Happens |
|---|---|
| Days 1–3 | ICU monitoring; chest tubes in place; pain management |
| Days 4–7 | Transfer to surgical ward; chest tubes removed; begin ambulation |
| Week 2 | Discharge (typically day 7–10); return home with oral medications |
| Weeks 3–6 | Gradual activity increase; fatigue is normal; breathing improves steadily |
| Weeks 6–8 | Most patients cleared for light activity; follow-up imaging |
| Month 3 | Most patients fully recovered; begin adjuvant chemotherapy if planned |
EPP Recovery Timeline
| Timeframe | What Happens |
|---|---|
| Days 1–5 | ICU; adaptation to single-lung breathing begins |
| Days 5–14 | Gradual transfer out of ICU; significant respiratory work |
| Weeks 2–4 | Hospital stay typically 10–14 days; discharge when stable |
| Weeks 4–12 | Longer recovery period; energy levels lower due to reduced lung capacity |
| Month 3 | Activity levels stabilizing; pulmonary rehabilitation helpful |
What Helps Recovery
- Pulmonary rehabilitation, particularly important after EPP; breathing exercises, graded exertion
- Physical therapy, maintaining strength and mobility during recovery
- Nutritional support, adequate protein and calorie intake accelerates healing
- Pain management, thoracic surgery involves significant incision; adequate pain control enables deeper breathing and faster recovery
- Caregiver support, at-home support for the first 4–6 weeks is essential for both P/D and EPP patients
Leading Mesothelioma Surgery Centers in 2026
Where you have surgery matters enormously. Surgical mortality, complete cytoreduction rates, and long-term survival are all significantly better at high-volume specialist centers.
| Center | Location | Key Specialty |
|---|---|---|
| Mount Sinai (Dr. Raja Flores) | New York, NY | P/D, 2026 landmark study; 0% 30-day mortality |
| MD Anderson Cancer Center | Houston, TX | All surgical approaches; largest trial portfolio |
| Brigham and Women’s Hospital | Boston, MA | EPP and P/D; trimodal protocol pioneers |
| Memorial Sloan Kettering | New York, NY | P/D and peritoneal surgery |
| Moffitt Cancer Center (Dr. Jacques Fontaine) | Tampa, FL | Minimally invasive robotic P/D |
| Penn Medicine / Abramson Cancer Center | Philadelphia, PA | Surgery + immunotherapy trials |
| University of Chicago | Chicago, IL | Peritoneal surgery + immunotherapy |
| Washington Cancer Institute | Washington, DC | CRS-HIPEC pioneer (Dr. Paul Sugarbaker) |
Most centers offer remote/telemedicine consultations. If you’ve been told surgery isn’t an option, you do not need to travel to get a specialist opinion, a remote review of your imaging and pathology can be arranged quickly.
Surgery and Your Legal Compensation Rights
Every mesothelioma patient who is a surgical candidate, and every patient who undergoes surgery, has full legal rights to pursue compensation from the asbestos manufacturers responsible for their disease.
Surgery does not affect your legal claim. In fact, a surgical case often results in higher total compensation because:
- Surgical costs are significant, EPP and P/D each cost $50,000–$150,000+ depending on the center, adding directly to documented economic damages
- HIPEC procedures cost $60,000–$200,000, directly billable as compensable medical expenses
- Pre-surgical chemotherapy and immunotherapy add further documented costs
- The physical severity of a surgical mesothelioma case, the loss of a lung, the recovery burden, the long-term lifestyle impact, often results in higher pain and suffering awards from juries
| Compensation Source | Amount |
|---|---|
| Personal Injury Lawsuit Settlement | $1M – $1.4M average |
| Trial Verdict | $5M – $11.4M average |
| Asbestos Trust Funds | $300K – $400K combined |
| VA Benefits (veterans) | $4,158+/month |
| Combined Total | $1.5M – $2M+ |
Your legal claim runs completely parallel to your medical treatment, including surgery. You can be recovering from a P/D procedure while your attorney is simultaneously filing your lawsuit and trust fund claims.
Questions to Ask Your Surgeon Before Mesothelioma Surgery
Bring these to your consultation:
- Do you recommend EPP or P/D for my case, and why?
- How many mesothelioma surgeries do you perform each year?
- What is your personal mortality rate for this procedure?
- What imaging and staging workup have been completed before your recommendation?
- Would you recommend neoadjuvant chemotherapy or immunotherapy before surgery?
- What adjuvant treatment will follow surgery?
- Will this be a standard P/D or extended P/D (with diaphragm/pericardium removal)?
- Am I a candidate for minimally invasive or robotic-assisted surgery?
- What clinical trials are available at your center that include surgery?
- If I was told surgery isn’t an option elsewhere, what specifically in my case leads you to a different conclusion?
Frequently Asked Questions
What is the difference between EPP and P/D surgery?
EPP (Extrapleural Pneumonectomy) removes the entire lung along with the pleural lining, diaphragm, and pericardium. P/D (Pleurectomy/Decortication) removes only the pleural lining and visible tumors while preserving the lung. P/D is now preferred at most major centers due to lower surgical mortality, better quality of life, and comparable or superior survival outcomes.
Is mesothelioma surgery safe in 2026?
At experienced, high-volume centers with carefully selected patients, yes. The 2026 Mount Sinai study demonstrated 0% in-hospital and 0% 30-day mortality for P/D patients who were properly selected and received imaging-guided surgical planning. At lower-volume or general centers, surgical mortality remains higher, which is why center selection matters enormously.
How do I know if I’m a candidate for surgery?
You need evaluation at a specialist mesothelioma surgical center, not a general hospital. The key factors are your cell type (epithelioid is most favorable), disease stage (1–2 preferred), performance status, lung and cardiac function, and imaging results. Even if you’ve been told you’re not a candidate elsewhere, a specialist opinion may reach a different conclusion.
What is the survival rate for mesothelioma surgery?
P/D combined with chemotherapy achieves median survival of 20–26 months. Trimodal therapy (P/D + chemo + radiation) achieves 26–31 months at top centers. For peritoneal mesothelioma treated with CRS-HIPEC, median survival reaches 44–53 months with 5-year survival rates of 47–65% in optimal candidates.
Can I still file a legal claim if I have surgery?
Absolutely. Your legal rights are completely unaffected by whether or how you’re treated medically. A surgical case often results in higher compensation because surgical costs are significant documented economic damages. Your attorney pursues your claim simultaneously with your treatment.
What is HIPEC and when is it used?
HIPEC (Hyperthermic Intraperitoneal Chemotherapy) is a heated chemotherapy treatment delivered directly into the abdominal cavity during surgery, used specifically for peritoneal mesothelioma. It is combined with cytoreductive surgery (CRS) and achieves 5-year survival rates of 47–65% in optimal candidates.
Should I get a second surgical opinion?
Yes, always. Mesothelioma surgery decisions carry life-altering consequences. If you’ve been told surgery isn’t possible, or if you’ve been offered EPP when P/D may be appropriate, a second opinion from a specialist center costs nothing and may significantly change your treatment path and your long-term outcome.
Surgery Is a Decision That Deserves a Specialist’s Eyes
The 2026 data is clear: for the right patients, mesothelioma surgery, performed by the right surgeon, at the right center, with the right patient selection protocol, achieves outcomes that chemotherapy or immunotherapy alone cannot match.
It is also a decision that depends entirely on your specific diagnosis, your cell type, your stage, your physical condition, and your goals. No general article can tell you whether surgery is right for you. Only a mesothelioma specialist can do that.
And while you’re making these medical decisions, the firms connected through this site are ready to pursue the full legal compensation your family deserves, from manufacturers who knew asbestos was lethal and kept selling it anyway.
⏰ Statutes of limitations are strict. Pursue your medical options and your legal rights simultaneously.
👉 Mesothelioma Compensation for Family Members: Spouse, Children & Dependents Guide 2026
About the Author
Brian Watson is a senior research editor at MesotheliomaLegalHelp.info with over eight years of experience covering legal and medical topics for digital health publications. He specializes in asbestos litigation, occupational disease, veterans’ benefits, and mesothelioma treatment research. Brian’s work is reviewed against current medical literature, legal precedent, and publicly available case data before publication. He holds a degree in journalism with a concentration in health and science writing.